Science of Breathing
Understanding the physiological behind the Nervous System.
This is the bridge between how you breathe and how your system responds. Clear, practical, measurable
Your nervous system has two branches
Fight. Flight.
Adrenaline and cortisol prepare the body for action.
Rest. Recover.
The body downregulates. Digests. Repairs. Restores.
Most people get stuck in sympathetic activation. Conscious breathing teaches your nervous system to switch between these states on demand.
How breathing changes your body
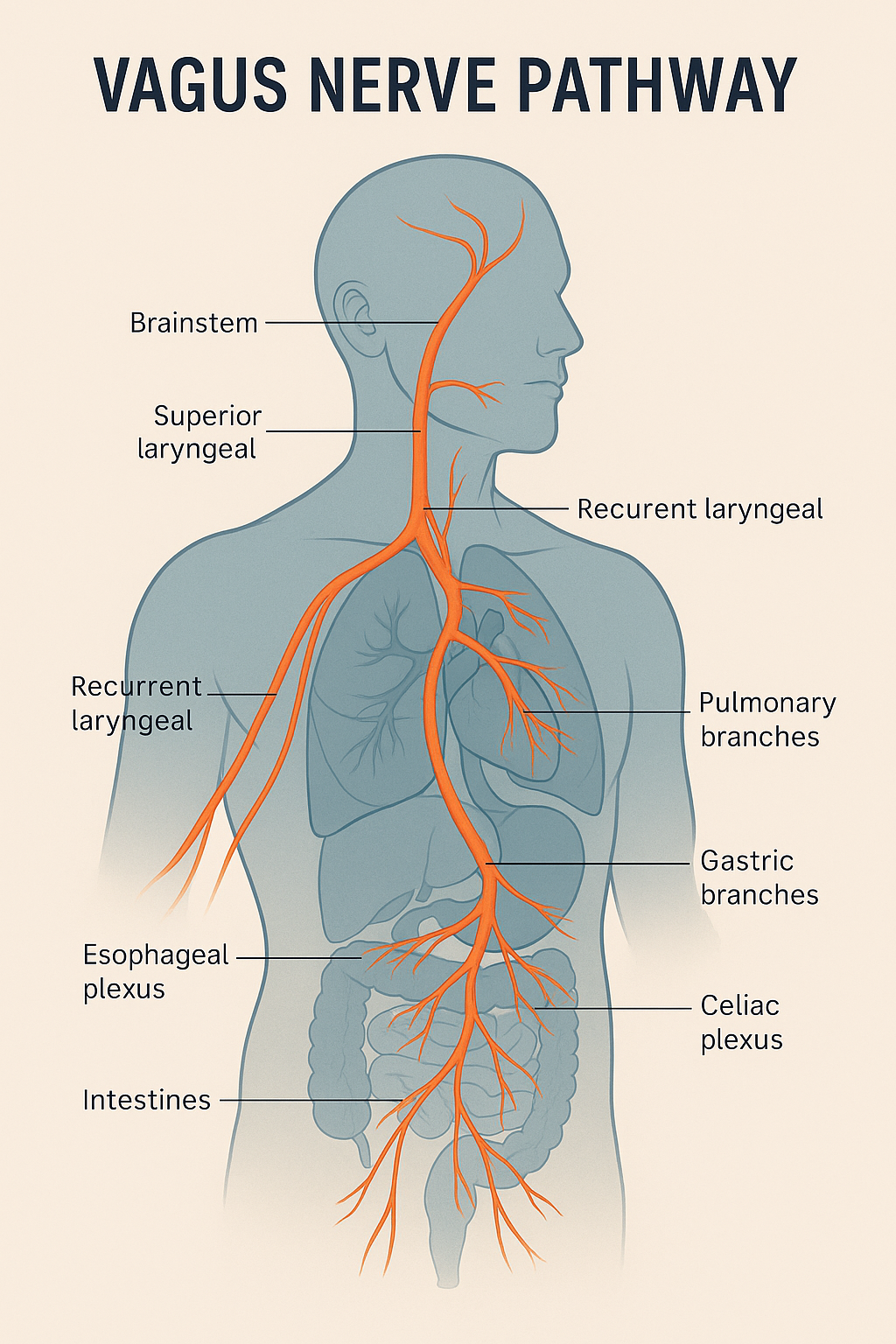
Vagal activation
The vagus nerve links brain and body. Belly-led breathing and longer exhales stimulate this pathway. Vagal activity rises. Stress hormones drop. One signal. The whole system shifts.
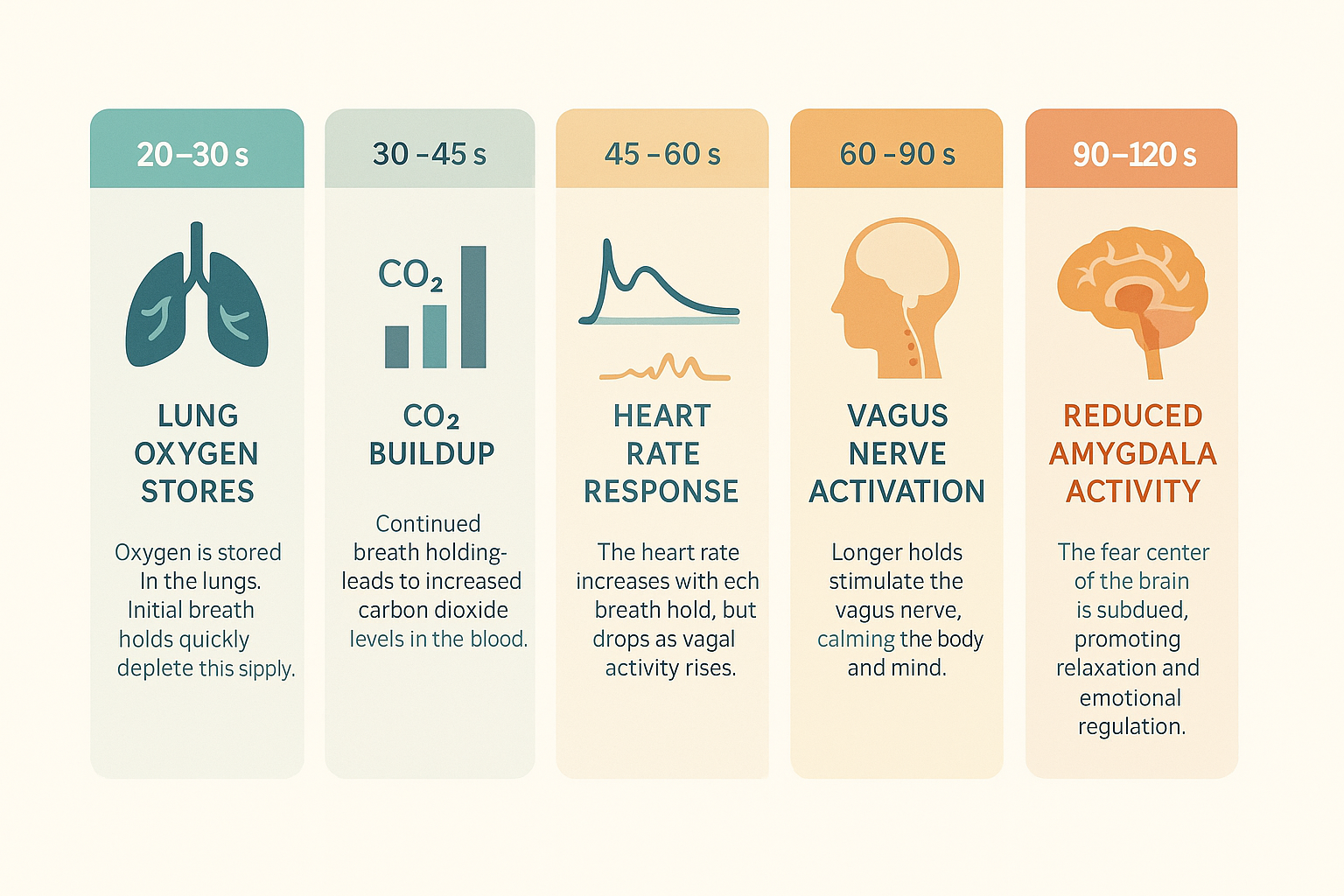
Controlled stress. Adaptation.
Breath retention creates controlled stress. You practice staying calm while stressed. The prefrontal cortex stays online and you learn regulation under load.
The sequence:
- Rapid breathing lowers CO2.
- The hold lowers oxygen.
- You remain present.
- The prefrontal cortex stays engaged.
- Recovery breathing activates parasympathetic.
Your body learns: I can handle this.

Carbon dioxide signal
CO₂ is not just waste. It is a regulator. Untrained, rising CO₂ can trigger panic. With practice, your body learns that a rise in CO₂ is information, not danger.
Training changes the meaning of the CO₂ signal.
Your nervous system rewires itself
More flexible. Activation and recovery on demand.
Faster recovery from stress.
Lower baseline cortisol.
Better heart rate variability.
More resilient immune system.
Higher stress tolerance. Presence in discomfort without shutting down.
This is not just how you feel. This is neural and endocrine reorganization.
Why breathing works.
Breathing is the only involuntary function you can voluntarily control. Change your breathing pattern, and you change everything downstream:
The physiological chain
Breath is the first move. Each step that follows can be trained and measured.
The way you breathe sets the tempo for the whole system. Fast, shallow breaths signal threat. Slower, steady cycles tell the body that it is safe enough to downshift.
When CO₂ rises, hemoglobin releases more oxygen into your tissues through the Bohr effect. This improves oxygen delivery, steadies energy, and helps the nervous system shift out of threat. Slow breathing keeps CO₂ at a level that supports oxygen uptake instead of blocking it.
Slow, controlled breathing increases vagal tone. This boosts parasympathetic activity, lowers heart rate, and signals the body that it can move out of stress mode.
Breath changes the balance between your fight-or-flight and rest-and-recover systems. Longer exhales reduce sympathetic drive and bring the body back toward regulation.
Fast breathing increases adrenaline and raises alertness. Slow, steady breathing reduces cortisol and shifts the body toward recovery and repair.
Breath directly controls heart rate through respiratory sinus arrhythmia. Slow breathing increases HRV, which reflects resilience and the ability to adapt under pressure.
Regulated breathing reduces chronic inflammation and supports immune function by lowering stress hormones and improving vagal activity.
Breath rhythm changes neural activity. Slower cycles increase prefrontal control and reduce limbic reactivity, improving focus, decision-making, and emotional stability.